>Corresponding Author : Joseph M Dutner
>Article Type : Research Article
>Volume : 4 | Issue : 2
>Received Date : 12 March 2024
>Accepted Date : 23 March 2024
>Published Date : 27 March 2024
>DOI : https://doi.org/10.54289/JDOE2400109
>Citation : Dutner JM, Sidow SJ, Cervero RM and Soh M. (2024) Endodontic Competence of the New General Dentist as Conceptualized by Predoctoral Educators: A Qualitative Exploration. J Dent Oral Epidemiol 4(2): doi https://doi.org/10.54289/JDOE2400109
>Copyright : © 2024 Dutner JM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Research Article | Open Access | Full Text
1Professor for Endodontics, US Army Postgraduate Dental School, Uniformed Services University of the Health Sciences, Joint Base Lewis-McChord, WA
2Clinical Associate Professor and Director, Postgraduate Program in Endodontics, Marquette University School of Dentistry, Milwaukee, WI
3Professor and Deputy Director, Center for Health Professions Education, Uniformed Services University of the Health Sciences, Bethesda, MD
4Assistant Professor for Health Professions Education, Uniformed Services University of the Health Sciences, Bethesda, MD
*Corresponding author: Joseph M Dutner, Professor for Endodontics, US Army Postgraduate Dental School, Uniformed Services University of the Health Sciences, Joint Base Lewis-McChord, WA
Abstract
Introduction: Without a unified standard for what constitutes endodontic competence for the new general dentist, predoctoral endodontic directors (PEDs) are left with the great responsibility of educating their learners in a manner that they believe best serves patients. Given different influencing factors and varying amounts of resources, these PEDs must ensure the achievement of meaningful objectives utilizing conceptual frameworks of competence. It is essential for dental educators and other stakeholders to gain an understanding of what current endodontic competence means to enable more accurate needs assessments to advise future curriculum development. The purpose of this study was to explore how endodontic competence for the new general dentist is conceptualized by predoctoral endodontics directors and their respective institutions while identifying perceived facilitators and barriers to its achievement.
Methods: Following the development of a semi-structured interview guide and its piloting, qualitative interviews were conducted with 10 PEDs. Interviews were transcribed and coded. The constant comparative method was utilized for data analysis.
Results: Interviews were conducted until thematic saturation was achieved. Conceptualization of endodontic competency seemed to be informed by three primary themes: the existing paradigmatic approaches of PEDs and their institutions, their concerns regarding validity evidence especially as it related to assessment, and the presence of institutional and logistical barriers.
Conclusion: Despite differences between their institutional definition and personal conceptualization of endodontic competence, PEDs report success at graduating new general dentists competent in endodontic diagnosis, case difficulty assessment, palliative treatment, and routine non-surgical root canal therapy on single-canal teeth of minimal difficulty.
Keywords: Endodontics; Undergraduate Dental; Competency based education; Teaching Assessment; Teaching Effectiveness
Abbreviations: PED: Predoctoral Endodontic Directors, AAE: American Association of Endodontists, CDAF: Case Difficulty Assessment Form
Introduction
Endodontics is the field of dentistry responsible for preventing and managing diseases of the dental pulp and the periapical tissues surrounding the roots of teeth, diseases that are responsible for 85% of all dental emergencies [1]. The majority of root canal procedures in the United States are performed by general dentists who may practice unrestricted within the full scope of dentistry following the completion of a 3-4 year curriculum in dental school and successful completion of a one-part comprehensive Integrated National Board Dental Examination (INBDE) and a clinical examination for licensure administered by a testing agency [2]. These clinical examinations rely solely on simulated exercises to measure the ability of the examinees to perform endodontic therapy, and none of them require complete treatment on premolars or molars, which are the teeth most commonly requiring non-surgical root canal therapy. Since only two states within the USA require a postgraduate residency to gain licensure, the predoctoral endodontics director (PED) must bear the burden of ensuring dental schools honor their societal obligation to graduate dentists who can demonstrate the competence to manage endodontic disease [3].
A universal definition of competence within the dental professions has yet to be realized, but common features include the “combination of knowledge, skills, professional attitude, personal attributes, an ability to work independently (without direct supervision), and context” [4]. However, skills associated with endodontic competence for the new general dentist (a dentist who has recently graduated from dental school and has not completed any additional post-graduate training) remain vague. For example, the American Dental Education Association states that endodontic competence as required for the new general dentist includes the ability to:
“Diagnose, identify, and manage pulpal and periradicular diseases” [5].
The Commission on Dental Accreditation, however, states that dental schools should train students to be:
“competent in providing oral health care within the scope of general dentistry, as defined by the school [emphasis added], including … pulpal therapy ...” [6].
In contrast, the American Association of Endodontists’ (AAE) whitepaper on endodontic competency describes the requisite skills of practicing dentists who diagnose and perform endodontic treatment, emphasizing the ability to:
“Use the AAE Case Difficulty Assessment Form (CDAF) to establish a rationale for appropriate treatment and or assess the need for referral due to anticipated case complexity” [7].
Additionally, according to the ADEA’s published 2020 Senior Student Survey, more than a third of respondents believed that their clinical experience gained in endodontic therapy during dental school was inadequate [8], an opinion shared by the majority of PEDs surveyed in 2014 [9]. The average graduate at the time of the study completed less than six root canal treatments on live patients. This shortage of patient experiences may explain why 36% of these same educators felt that their graduates were not competent to perform molar endodontic treatment in their practices [9]. These findings are particularly concerning as two-thirds of new dentists believe their training was adequate even though over a third of their faculty believe they are incompetent at performing molar endodontic treatment. For new dentists who lack endodontic competence, their treatment decision-making may favor other modalities to manage pulpal and periapical disease, including the unnecessary extraction of sustainable teeth.
With professional and accrediting bodies lacking clear directives for endodontic competency, it is not surprising that there are incongruencies between the involved stakeholders. Dental schools, PEDs, dental students, general dentists, and patients have different motivations and perspectives that influence how they construct their concepts of competence. However, as the individuals responsible for the training of new general dentists in tooth-saving root canal procedures, PEDs provide some of the most valuable insight into what endodontic competence means for the general dentists currently entering practice. As with most modern professional schools, the addition and deletion of content has the potential to produce individuals with different levels of competence than their predecessors. Through the exploration and comparison of PEDs’ perspectives, a more fruitful needs assessment can inform both predoctoral and post-graduate curriculum development.
As a conceptual framework, we applied Kern’s six-step approach to curriculum development. In this approach, the first step includes a general needs assessment [10]. A general needs assessment is initiated with an investigation into the current approach utilized to solve a problem. Once the current approach is identified, we then begin to explore ideal approaches to solving said problem. Any gap between the current and ideal curricular approaches reveals the general needs. The general needs assessment serves as the foundation for subsequent curriculum design and development, including a more targeted needs assessment, goals and objectives, educational strategies, evaluation and feedback, and implementation.
As health professions educators, we have an ethical obligation to act in the public’s best interest as it relates to safety in healthcare. With an evolved needs assessment, a more effective curriculum design will better serve society. Thus, the purpose of this research was to explore how endodontic competence for the new general dentist is conceptualized by predoctoral endodontics directors and their respective institutions while identifying perceived facilitators and barriers to its achievement.
Materials and Methods
This study was approved by the Institutional Review Board (IRB) for the Uniformed Services University of the Health Sciences (Protocol DBS.2021.294).
Potential participant PEDs were recruited from within three separate regions, roughly corresponding to regional licensing exams. Participant recruitment was completed through internet discussion group postings, e-mail invitations, and snowball enrollment methods.
Although an initial semi-structured interview guide was developed, emerging themes influenced further revision of the interview guide. Interview questions did not collect personal or institution-identifying information. While the guide did request some basic quantitative information pertaining to the dental school’s enrollment, curriculum, and specific requirements or assessments, open-ended questions primarily focused on individual concepts regarding endodontic competence, perspectives of their institutions’ formal and informal definitions of such competence, their beliefs on the competence of their graduates, and perceived challenges and best practices.
Interviews were conducted by the principal investigator and transcribed using Transcription Hub (Issaquah, WA) transcribing service. After the accuracy of the transcriptions were verified, interview recordings were deleted.
QDA Miner Lite (Provalis Research, Montreal, Canada) and NVIVO 12 (Lumivero, Denver, CO) were utilized to analyze the interview transcripts. All investigators participated in identifying and coding for emerging themes. A thematic analysis was completed with the constant comparative method to explore the relationship between themes that emerged during the interviews with those that have been previously identified [11].
Results
After thematic saturation was achieved, member checking was performed to confirm identified themes. In total, ten participants were interviewed, distributed among all geographic regions from schools both with and without advanced education programs in endodontics. Considering that the total number of active PEDs within the US and Canada is approximately 71 educators, the final sample of 10 participants represented the desired diversity and adequate representation (14% of the population).
Four content domains were identified by PEDs, along with their institutions, as the ideal conceptualization of endodontic competence: endodontic diagnosis, case difficulty assessment, palliative treatment, and routine non-surgical root canal therapy on single-canal teeth of minimal difficulty. This idealized approach to endodontic competence for the new general dentist was informed by critical facilitators and barriers that reside at all levels of dental education – individual, programmatic, and institutional. The following three themes were identified and weave in the previously mentioned four content domains (see Figure 1):
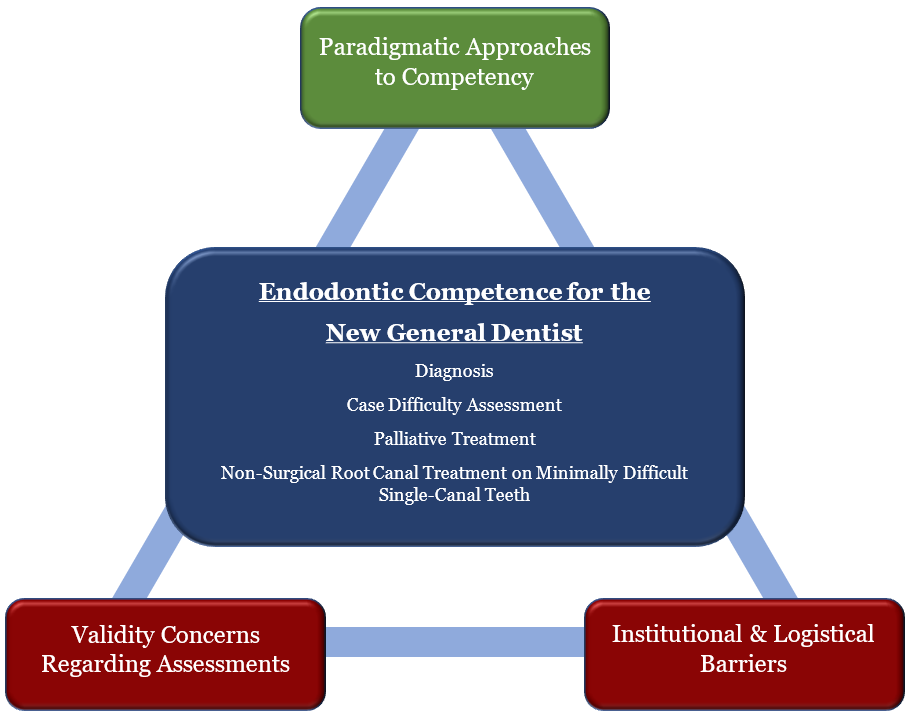
Figure 1: Defining Endodontic Competence for the New General Dentist
Theme 1: Paradigmatic Approaches to Competency
When asked to describe their institution’s definition of “competence in pulpal therapy,” several participants listed some combination of numerical case requirements and competency assessment examinations. The format of the competency assessments varied among the responses. The most common assessment was the independent performance of non-surgical root canal therapy on a live patient, but some participants also described a pre-clinical exercise on extracted or plastic teeth like that required for the licensing board examinations. When institutional definitions articulated competence as individual endodontic skills, they were listed as complete procedures (e.g., non-surgical root canal therapy on an anterior tooth, pulpotomy on a molar tooth, etc.) rather than the individual integral component skills (e.g., determining working length, obturation, etc.).
In general, when asked about their individual definition of “competence in pulpal therapy,” participants described specific knowledge, skills, and abilities spanning several domains related to the practice of endodontics. These ranged in specificity from broad descriptions of general endodontic knowledge to well-defined procedures. Commonly identified aspects of competence were the ability to diagnose endodontic pathosis, perform a case difficulty assessment, and provide emergency palliative services to relieve pain. Some participant went on to define competence as the technical completion of uncomplicated root canal procedures on anterior and/or premolar teeth. As one example, a participant described endodontic competence as being able to:
“... formulate an accurate diagnosis. Non-molar endo… that falls within the guidelines of that AAE case difficulty form. They need to know and refer, refer truthfully…non-molar endo. Really anterior, maybe only.” – PED 9
Additional representative quotations further delineating the individual and institutional approaches to endodontic competence can be found in Table 1.
Table 1: Definitions of Competence
| “In the fourth year, they have to choose one case for competency that they do from start to finish but they’re supervised by their general faculty on their floor. And that is their competency…one either anterior or premolar, minimal difficulty case, and they also have one pulpotomy to perform for competency. That’s all we have.” |
| “In addition to diagnosis, they need to be able to treat endodontic conditions…we include vital pulp therapy as part of that, at least recognize and know how to manage it…be able to do perform root canal treatment, get patients out of pain, refer as needed, recognize which kind of cases fall within the scope of the general practitioner. And so that's kind of the broad scope of it.” |
| “We have sort of a loose requirement of completing at least four cases. One of which needs to be a molar case, one of which is done as what we call CSA or Clinical Skills Assessment. It’s kind of their test case, they need to complete it without any significant assistance from the faculty to demonstrate to the faculty that they can manage a straightforward endodontic case…they are also required to do a case presentation to one of the faculty members, where they basically walk through the case, and the faculty quizzes them on basic information…just to get the feel…do they really have a significant competency that we feel we can sign off on?” |
| “The student will actually perform a start-to-end treatment without any faculty oversight. They will have to show that they can achieve a competent outcome without the faculty supervision and advice…they have to do one of those.” |
| “They have a patient clinical competency on either their third or fourth case. And we also have a bench test competency that they need to pass and also the OSCE competency. So I guess our definition is, are they able to pass those? Can they do well on the exam and show that they can apply what they learned?” |
| “The student needs to be competent in the diagnosis of pulpal pathosis. They need to know the goals of the treatment and then how to perform the treatment.” |
| “…the ability to work independently in non-surgical root canal therapy, non-molar treatment.” |
| “…non-surgical root canal therapy on non-molar endo start to finish without faculty involvement.” |
| “…to be able to formulate an accurate diagnosis. Non-molar endo…that falls within the guidelines of that AAE case difficulty form. They need to know and refer, refer truthfully…non-molar endo. Really anterior, maybe only.” |
| “…being able to know your limitations is the number one thing that I try to teach…knowing cases that are too difficult…having the judgment to say, ‘Wait. Let me refer this.’…being able to diagnose properly, being able to, at the minimum, get a patient out of pain…being able to do straightforward cases well. So cases that are fun and not challenging, I think they can do it. …it’s all about case selection too.” |
| “Their role as general dentist is to really know how to diagnose and to give urgent care. And from that point forward, they really need to be referred to an endodontist.” |
| “I think the philosophy we have here is being able to treat a very straightforward initial case on an anterior premolar makes sense. Also, to be able to potentially do an emergency procedures such as a pulpotomy or pulpectomy on a molar, and so I think that that's what a good general dentist who's starting out should be able to do on their own you know. And then also be able to recognize those cases that they need to refer.” |
| “I think it’s the ability…to really diagnose, I don't think necessarily treat the case, but diagnosis and refer as appropriate. I think that's more what they should be doing instead of just thinking about cleaning and shaping with the new files quicker and they're done. So I think the diagnosis is the more important portion for us in pulpal therapy for them to be competent.” |
| “I think I would say someone is competent, when number one, they can select a case that fits within their level of experience and their level of knowledge. And that they can complete the case with an outcome that meets the standards that our profession dictates, and then they can manage that case, after the fact…I kind of like to see it in a big picture format, that it's not just the mechanics of doing conventional root canal therapy. It's everything that leads up to it: selecting the case, making the proper diagnosis…getting good profound anesthesia, good isolation, and technically doing the root canal therapy within the standards that they've been trained and then restoration and then the recall afterwards.” |
Theme 2: Validity Concerns Surrounding Competency Assessments
One participant described a two-week delay for one dental student’s graduation to allow them to achieve their institution’s requirements to demonstrate competency. However, when asked to approximate the percentage of graduates that were competent in non-surgical root canal therapy, the estimates ranged from 50-99%, 40-90%, and 0-75% when treating anterior teeth, premolars, and molars, respectively. Even though only a couple of interviewees stated so explicitly, it can be surmised from these numbers that the formal methods of competency development and assessment within their institutions were not seen as reliable. When this discrepancy was noted by a specific response, it was often attributed to the number of cases required for competency development. The number of cases of endodontic live patient encounters that the institutions considered required for competency in pulpal therapy varied between two and four.
“I find it hard to say somebody is competent after four cases.” – PED 6
“I don't think with the 3 that we are doing right now or 4, I don't think they're competent to really do pulp therapy out there.” – PED 5
Some participants also commented directly on the content validity of their institutions’ current assessments of competency. Although all participants described the practice of competency assessments evaluating independent performance of non-surgical root canal therapy, some preferred that these assessments focused more on diagnosis, emergency treatment, and facilitating effective referrals to the endodontic specialist.
“So the competency [assessment], in my opinion, needs to focus way more on the piece of diagnosis, knowing how to do a pulpotomy or pulpectomy utmost, knowing when and how to prescribe antibiotics, and when it's indicated, and focusing on that piece of the communication between the dentist and the endodontist.” – PED 8
Theme 3: Institutional and Logistical Obstacles
There was general agreement among the participants about obstacles to developing competency in their learners. The most common challenge involved the lack of available time within the dental school curriculum in which faculty were able to interact with their learners.
“I think it's the time that we spend with them. I think we should have more time… we don't have enough time in the curriculum for them to be competent, because they have to do all the other competencies and learn all of this.” – PED 5
Although there was one outlier, the rest of the participants concurred that the number of faculty within their institutions was inadequate given the number of students, which varied between 65 to 235 students per class.
“It's really difficult to do all of this with just two faculty. You know, I have to teach all the courses, I have to cover the clinic, and then I have all the other school functions that I have. It’s really daunting.” – PED 4
“There are too many students. There are too many students, not enough faculty… you always have a student that you know, is shy or isn’t gonna ask for help, and they kinda have a tendency to get lost… I go after hours at night for kids that were struggling and work with them just because this was it. If they didn't get it sophomore year, that was it. Then, they saw patients. That's really scary.” – PED 9
Another identified challenge was the length of time between their learners’ clinical endodontic experiences. They described this gap in endodontic practice as resulting in an evident loss of knowledge over time.
“But during their third year, they had zero interaction with us, zero. And it ended up being like they're doing such a rigorous course in the second year, but then they're not doing anything during the third year. And then when they come into clinic in their fourth year, they know nothing. It's as if we are starting fresh.” – PED 8
“I think that the time between cases is problematic…they may do all their preclinical stuff, and then they might not do a root canal for over a year… or they'll do one, and then they won't do one for three months and forgot what they did last time and so forth… if it's something that you only look at once every couple of months, then they tend to lose what they had knowledge-wise and so that repetitive reinforcement is lacking just by the nature of the institution.” – PED 7
Discussion
Our study aimed to explore how PEDs and their institutions conceptualize endodontic competence for the new general dentist. Conceptualization of endodontic competency was grounded in four distinct curricular domains and shaped by three primary facilitators and/or barriers: existing paradigmatic approaches of PEDs and their respective institutions, concerns regarding validity evidence especially as it related to assessment, and the presence of institutional and logistical obstacles.
It was interesting to note that most participants described their institution’s definition of competence in a quantitative manner regarding the ability to complete a certain number of endodontic cases and/or specific assessments. This finding is consistent with previous survey results in which 85% of responding PEDs reported having live patient competency examinations at their institutions, but our participants reported their institutions’ case numerical requirements were less than the survey’s average of 4.9 root canal treatments [9]. This concept of competence differed from the educators’ interpretation, which included cognitive and technical skills. For example, the ability to diagnose endodontic disease and assess the endodontic case difficulty were the most described skills required for the educators’ concept of competence. While the educators’ approach to competency reflected specific activities associated with the successful overall management of the endodontic patient broken down into its component knowledge and skills, the institutional approach was described in a more disconnected manner focusing merely on the completion of standardized procedural requirements without much further context.
The implications of these paradigmatic differences are most evident when considering the methods of assessing learners’ endodontic competency. The validity of the described “competency” assessments is difficult to reconcile with the overwhelming faculty perception that many, and in some cases, most of their graduates were not competent in several aspects of non-surgical root canal therapy. Interestingly, most of the assessments were not specifically concerned with the faculty’s concept of what their graduates should be competent in. For example, several of the participants described their thoughts about how graduates should be competent in diagnosing endodontic disease and assessing case difficulty. Since most of the live patient encounters used as competency assessments were already curated based on diagnosis and case difficulty, these important concepts were not usually part of the assessment.
When viewing these findings while considering Messick’s validity framework, there are several sources of evidence that warrant further investigation [12]. There is occasional disagreement in content validity between the competency assessments and what the educators indicated should be assessed. For example, some participants explained that the assessments should focus on tasks of lower difficulty (e.g., diagnosis, case assessment, etc.) consistent with what they expected from new general dentists rather than independent performance of non-surgical root canal therapy. The consequential validity also deserves additional examination as only one participant described briefly holding back a learner from graduating due to their inability to complete their institution’s requirements for competency. This conflicted with their perceived percentage of graduates competent in endodontic therapy. The internal structure validity, or reliability, of the assessments also requires more study. For all the participants interviewed, the clinical competency assessment was limited to one clinical case performed independently. Most agreed that this was an inadequate number of assessment occasions to sample the learners’ abilities.
The most common barrier to achieving these competencies was the inadequate amount of time spent with learners. Dental schools in the United States mostly stick to a fixed-time curriculum. A student will be in and out of dental school in four years with little exception. Therefore, the onus of developing competent dentists in this limited time falls on the faculty educators who have little control of the amount of time available for each learner. One survey found that the average time dental students spent in didactic endodontic lectures and pre-clinical laboratory courses was 33.6 and 53.0 hours, respectively [9]. The same pre-COVID survey found that the average number of root canals performed was less than six [9]. Several faculty participants described achieving competency in this limited time as an almost impossible task in which they try the best they can, but in doing so, they admit the limitations of such a situation. Since such limited time in the clinic is available, there may be an implicit reliance on the general competency hypothesis, a theory introduced by Chambers stating that “dentistry is learned as a global set of skills, understanding, and values that manifests itself in various discipline-specific fashions when the circumstances call for that type of performance” rather than being learned as discipline (or specialty) -specific skills and competencies [13].
In combination with the limited time, the pace and consistency of a dental student’s educational experiences addressing specific competencies is often at odds with skill development. Deliberate practice, a learning theory introduced by Ericsson et al. (1993), describes the individualized training activities specially designed by a coach or teacher to improve specific aspects of an individual’s performance through repetition and successive refinement” [14], enabling a learner to address specific areas in which they can improve. A learner in dental school does not often have the luxury of creating a personalized plan with a dedicated clinical coach to enable deliberate practice for specific tasks. Rather, the learner must dedicate and focus their attention and learning to the immediate task at hand, which can manifest in any number of procedures and specialty areas during their rotations through the dental school clinics. Other learning theories explore the benefits of spaced, or distributed, learning versus mass learning [15,16]. By regularly spacing out educational experiences or specific types of clinical procedures, learners were able to demonstrate less skill degradation. Such distributed learning is hard to optimize when endodontic clinical skills are taught during a concentrated pre-clinical or didactic course, but an excessive amount of time elapses before or between live patient clinical encounters.
While several best practices were discussed in the interviews, future studies may benefit from determining the effectiveness and feasibility of said practices. For example, participants recommended developing an endodontic block rotation in which learners could focus on endodontic treatment for at least one week. This practice could enable more individualized skill development as the learners would be able to utilize feedback for each subsequent learning encounter without as much concern over skill and knowledge degradation. Another example was the establishment of endodontic study clubs for a limited number of students with a particular interest in endodontics, allowing further clinical encounters towards the achievement of competency.
This study had several limitations. First, our recruitment may have been influenced by self-selection bias. Although attempts were made to recruit a diverse group of educators, it is likely that those willing to participate in this research were particularly dedicated to the advancement of endodontic education. Second, there are several stakeholders invested in the endodontic competence of new dental school graduates. Administrators and educators within the dental school, professional dental organizations, accrediting bodies, new dentists themselves, and the public are just some of those who could contribute significantly to the understanding of this topic. Third, specialist dental educators may have elevated concepts of competence within their own field beyond what can be reasonably expected of general dentists. Although this is a potential source of bias, it is also noteworthy that general dentists and endodontists alike are held to the same standards of practice [16,17].
Conclusion
There is not a single, agreed-upon definition of endodontic competence for the new general dentist. When considering their individual concepts of such, the PED’s in this study described success at graduating new general dentists competent in diagnosis, case difficulty assessment, palliative treatment, and routine non-surgical root canal therapy on single-canal teeth of minimal difficulty even as they challenged the validity of their institutions’ assessments of competency. They are managing this challenging task while facing an inadequate number of faculty, limited patient pools and subsequent clinical encounters, and severe, unrelenting time constraints. Developing endodontic competence that further bridges the gap between current and ideal concepts by including premolar and molar endodontic therapy may require additional postgraduate dental education that provides concentrated blocks of endodontic patient encounters under close mentorship with endodontic educators.
Acknowledgements: The authors report no funding sources for this research.
Disclosure: The opinions and assertions expressed herein are those of the authors and do not reflect the official policy or position of the Uniformed Services University of the Health Sciences or the Department of Defense. The authors deny any financial, economic, or professional interests that may have influenced the design, execution, or presentation of this research.
References
- Hasler J., Mitchell D. 1963;Analysis of 1628 cases of odontalgia:a corroborative study. J Indianapolis Dist Dent Soc. 1963. 17(23):23–25. [Ref.]
- ADA Survey Center. The 2005–06 Survey of Dental Services Rendered. Aug. Am Dent Assoc. 2007. [Ref.]
- Chuenjitwongsa S., Oliver RG., Bullock AD. Competence., competency–based education., and undergraduate dental education:a discussion paper. Eur J Dent Educ. 2018;22(1):1–8. [PubMed.]
- ADEA Competencies for the New General Dentist. J Dent Educ. 2017;81(7):844–847. [PubMed.]
- Commission on Dental Accreditation. Standards for Predoctoral Dental Education [Internet]. Chicago., IL. 2020. [Ref.]
- American Association of Endodontists. Endodontic Competency White Paper [Internet]. Chicago. 2017. [Ref.]
- Istrate EC., Slapar FJ., Mallarapu M., Stewart DCL., West KP. Dentists of tomorrow 2020:An analysis of the results of the 2020 ADEA Survey of U.S. Dental School Seniors. J Dent Educ. 2021;26:85(3):427–440. [PubMed.]
- Woodmansey K., Beck LG., Rodriguez TE. The Landscape of Predoctoral Endodontic Education in the United States and Canada:Results of a Survey. J Dent Educ. 2015;79(8):922–927. [PubMed.]
- Thomas PA., Kern DE., Hughes MT., Chen BY., editors. Curriculum Development for Medical Education:A Six–Step Approach. 3rd ed. Baltimore:Johns Hopkins University Press. 2015. [Ref.]
- Grove RW. An analysis of the constant comparative method. Int J Qual Stud Educ. 1988;1(3). [Ref.]
- Messick S. Validity of psychological assessment:Validation of inferences from persons' responses and performances as scientific inquiry into score meaning. Am Psychol. 1995;50(9):741. [Ref.]
- Chambers DW. Preliminary evidence for a general competency hypothesis. J Dent Educ. 2001;65(11):1243–1252. [PubMed.]
- Ericsson KA., Krampe RT., Tesch–Römer C. The role of deliberate practice in the acquisition of expert performance. Psychol Rev. 1993;100(3):363. [Ref.]
- Cecilio–Fernandes D., Cnossen F., Jaarsma DA., Tio RA. Avoiding surgical skill decay:a systematic review on the spacing of training sessions. J Surg Educ. 2018;75(2):471–480. [PubMed.]
- Lee TD., Genovese ED. Distribution of practice in motor skill acquisition:Learning and performance effects reconsidered. Res Q Exerc Sport. 1988;59(4):277–287. [PubMed.]
- American Association of Endodontists. The Standard of Practice in Contemporary Endodontics. Colleagues for Excellence. Fall. 2014. [Ref.]
- Ian Watson. Canadian Academy of Endodontics. Standards of Practice. 2022. [Ref.]