>Corresponding Author : Hlaibi Omnia
>Article Type : Case Report
>Volume : 6 | Issue : 1
>Received Date : 22 Dec, 2025
>Accepted Date : 05 Jan, 2026
>Published Date : 24 Jan, 2026
>DOI : https://doi.org/10.54289/JCRMH2600101
>Citation : Omnia H, Hasnae S, Abdellah A, Houssin B, Sakher M, et al. (2026) Metrorrhagia Revealing Clear Cell Adenocarcinoma of the Uterine Cervix: A Case Report. J Case Rep Med Hist 6(1): doi https://doi.org/10.54289/JCRMH2600101
>Copyright : © 2026 Omnia H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Case Report | Open Access | Full Text
Gynecologic department, Centre Hospitalier Universitaire Ibn Rochd, Faculté de Médecine et Pharmacie, Université Hassan II de Casablanca, Casablanca, Morocco
*Corresponding author: Hlaibi Omnia, Gynecologic department, Centre Hospitalier Universitaire Ibn Rochd, Faculté de Médecine et Pharmacie, Université Hassan II de Casablanca, Casablanca, Morocco
Abstract
Cervical adenocarcinoma is uncommon, and the clear-cell subtype is rare.
The particularity of this observation lies in the absence of known factors predisposing to this type of cancer, as well as its rarity.
This is a young woman who reported metrorrhagia associated with leucorrhoea for three years, and whose examination revealed a five centimetres mass of the uterine cervix, Anatomopathological study of the biopsy revealed clear-cell tumour proliferation, A pelvic MRI showed a cervical mass can be classified IIIB according to FIGO classification.
The patient received courses of chemotherapy, radiotherapy and brachytherapy.
A follow-up pelvic MRI showed an almost complete response after treatment.
Through this observation, we emphasize the rarity of this type of adenocarcinoma and the need for research to improve its management.
Keywords: The Clear Cell Adenocarcinoma of the Cervix, Diethylstilbestrol, Rare Pathology
Abbreviations: DES: Diethylstilbestrol, HPV: Human Papillomavirus
Introduction
Cervical adenocarcinoma is uncommon, and the clear-cell subtype is rare [1].
The latter has a very poor prognosis [2].
In addition to in utero exposure to diethylstilbestrol (DES), genetic factors such as microsatellite repeat sequence instability, human papillomavirus (HPV) infection, bcl-2 protein overexpression, p53 gene mutation and exogenous risk factors other than DES exposure may play an important role [3].
The particularity of this observation lies in the absence of known factors predisposing to this type of cancer, as well as its rarity.
Clinical Observation
Thirty-five years old woman, married, menarche at 14 years, with antecedent fetal death in 2003, operated in 2017 for tubal impermeability (under laparoscopy), chronic smoker since 2015, with no history of Di-Ethyl-Stilboestrol treatment taken by her mother during pregnancy and no family history of gynecological cancer, who presented for tree years with metrorrhagia of moderate abundance with fetid leucorrhea associated with weight loss and asthenia.
General examination revealed an asthenic patient, with slightly discoloured conjunctivae. Gynaecological examination revealed a five centimetres mass of the uterine cervix reaching the proximal third of the vagina, with infiltration of the parametrium (figure 1).
Anatomopathological study of the biopsy revealed clear-cell tumour proliferation, with immunohistochemical studies showing positive anti-CK7 antibodies, diffusely positive anti-PAX8 antibodies and focally positive anti-CD10 antibodies, all in favour of a clear-cell carcinoma of the cervix
A pelvic MRI showed a cervical mass with discrete T2 hypersignal, diffusion hypersignal, T1 hyposignal, moderate and heterogeneous enhancement after injection of godalinium, measuring 57 x 40 mm and 55 mm in height, prolapsed into the vagina and responsible for infiltration of the proximal parametrium and the upper 1/3 of the vagina without pelvic lymphadenopathies; the ovaries were normal (figure 2).
The patient received twenty three sessions of radiotherapy (46 Gy) spread over one month, five courses of paclitaxel-carboplatin-based chemotherapy one week apart, and two sessions of brachytherapy.
A follow-up pelvic MRI showed an almost complete response after treatment (figures 3-4).
The patient is currently under clinical and radiological surveillance with pelvic MRI every six months.
Discussion
In recent decades, there has been a significant increase in the incidence of adenocarcinoma of the cervix, particularly in young women under thirty-five years [4]. Currently, adenocarcinomas account for 5-25% of cervical carcinomas [4,5]. They are classified by the OMS into five types, including clear-cell adenocarcinoma, which remains very rare [1,4]. In terms of etiopathogenesis, like squamous cell carcinoma, there is a significant association with HPV (Human Papilloma Virus), particularly with the HPV-18 subtype [6-8]. Nevertheless, and particularly in the case of clear-cell adenocarcinoma, since the 1970s, the work of Herbst and Noller has demonstrated the responsibility of diethylstilbestrol taken during pregnancy in the development of clear-cell adenocarcinoma of the cervix or vagina in girls from these pregnancies [9].
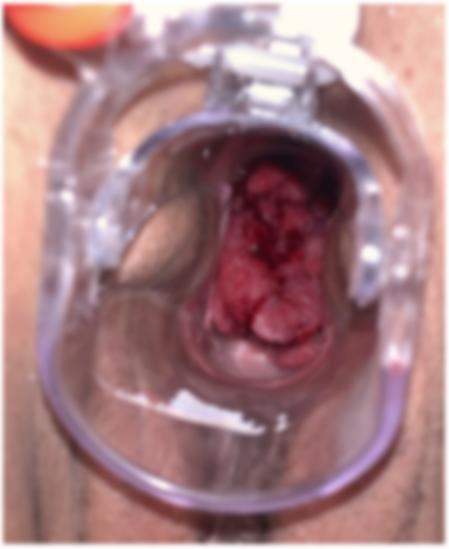
Figure 1. Speculum examination showing a five-centimetre cervical mass
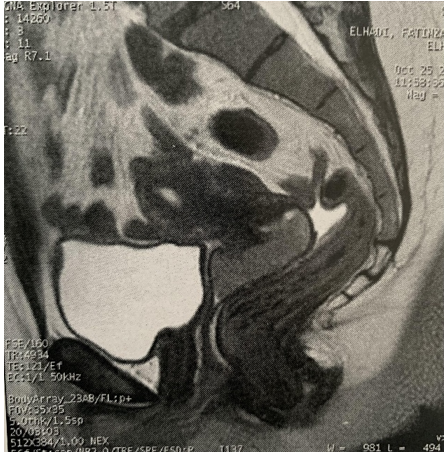
Figure 2. Prolapsed cervical mass in the vagina, responsible for infiltration of proximal parameters and the upper third of the vagina
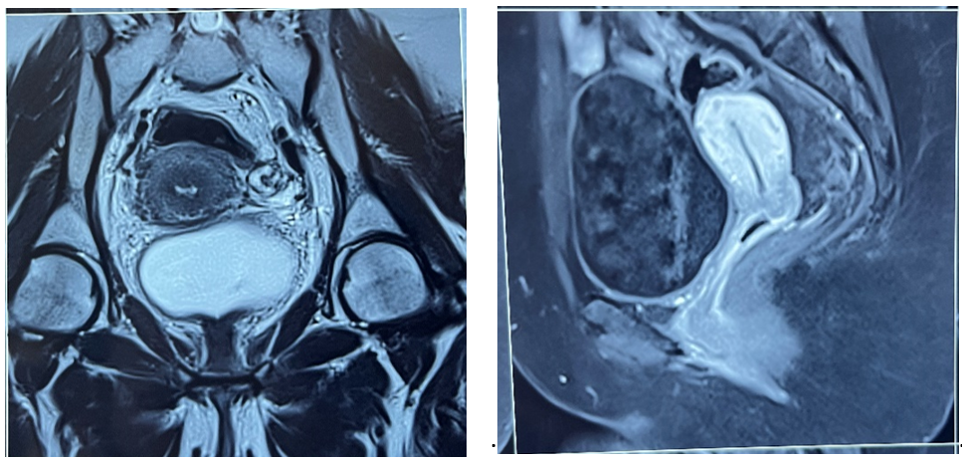
Figure 3-4: Control MRI (post concomitant radio chemotherapy + brachytherapy) showing almost complete response
This risk is higher for women whose mothers started DES before the 12th week of pregnancy, and persists from birth until the age of 34. Women exposed to DES in utero should therefore undergo regular cytological and colposcopic surveillance. However, in our case, the notion of in utero exposure to DES had not been found. This leads us to think of other risk factors not incriminated in this type of cancer, even though they play a crucial role in its carcinogenesis in the same way as other cancers, namely genetic predisposition. In fact, in the literature, cases of cervical adenocarcinoma have been reported in the same family, or young girls have presented with this type of cancer without any known detectable risk factor [10]. Consequently, it is necessary to suggest the presence of one or more genes responsible for this predisposition. It is necessary to develop the oncogenetics of cervical cancer, particularly clear-cell adenocarcinoma, in order to better elucidate its etiopathogenesis [10]. In our case, the patient refused the genetic study, which limits our observation.
As for its evolution, the majority of reported cases illustrate the very poor prognosis of this pathology, whereas in our case, the patient responded well to concomitant radio-chemotherapy plus brachytherapy and rigorous surveillance was established.
Conclusion
Cervical adenocarcinoma is uncommon, and the clear-cell subtype is rare, with a very poor prognosis.
In addition to in utero exposure to diethylstilbestrol (DES), there are other risk factors.
In contrast to squamous cell carcinoma, the etiopathogenesis is still poorly understood, which makes its management difficult, so we need more research in gynaecology, anatomopathology and oncology in order to establish a good codified management and thus improve the prognosis.
References
- Sami H., Eddaoualline H., S Barkiche., Elouarzazi S., Mazouz K., et al. Clear Cell adenocarcinoma of the Cervix Without Exposure to Diethylstilbestrol. World Journal of Pharmaceutical and Medical Research. 2020;6(2):29–31. [Ref.]
- Tantitamit T., Hamontri S., & Rangsiratanaku L. Clear cell adenocarcinoma of the cervix in second generation young women. Who are without maternal exposure to diethylstilbestrol: A case report, Gynecologic Oncology Reports. 2017;20:34–36. [PubMed.]
- Reich O., Tamussino K., Lahousen M., Pickel H., and Haas J. Clear Cell Carcinoma of the Uterine Cervix: Pathology and Prognosis in Surgically Treated Stage IB–IIB. Disease in Women Not Exposed in Utero to Diethylstilbestrol., Gynecologic Oncology. (2000);76(3):331–335. [PubMed.]
- Fetissof F. Anatomie pathologique des carcinomes infiltrants du col utérin. Encycl Méd Chir. Éditions scientifiques et médicales Elsevier SAS, Paris. Gynécologie. 2002;605–635:11. [Ref.]
- Lellan R M C., Dillon M B., Woodruff J D., et al. long term follow up of stage I cervical adenocarcinoma treated by radical surgery., Gynecol Oncol. (1994);52(2):253–9. [PubMed.]
- Fujiwara H., Follen Mitchell M., Arseneau J., et al. Clear cell tumor associated with human Papillomavirus– 18. Cancer. 1995;76:1561–1600. [PubMed.]
- Lynch HT & Reich JW. Diethylstilbestrol: genetics, teratogenesis and tumor spectrum in humans. Med Hypotheses. 1985;16:315–332. [PubMed.]
- Das BC., Gopakrishna V., Das DK., et al. Human papillomavirus DNA sequences in adenocarcinoma of the uterine cervix in Indian women. Cancer. 1993;72:147–53. [PubMed.]
- Villeret Julia., Verschuur., Sultan., Charles. Diethylstilbestrol exposure during pregnancy with primary clear cell carcinoma of the cervix in an 8–year–old granddaughter: a multigenerational effect of endocrine disruptors? Human Reproduction. 2020;267. [Ref.]
- Stalens JP., Maton P., Gosseye S., et al. Hemihypertrophy, bilateral Wilms ‘tumor and clear cell adenocarcinoma of the uterine cervix in a young girl, Med. Pediatr Oncol. 1993;21(9):671–5. [PubMed.]