>Corresponding Author : Safaa Mourabit
>Article Type : Case Report
>Volume : 4 | Issue : 3
>Received Date : 22 Jan, 2024
>Accepted Date : 06 Feb, 2024
>Published Date : 09 Feb, 2024
>DOI : https://doi.org/10.54289/JCRMH2400111
>Citation : Mourabit S, Mhaber S, Elkabli A, Barakat L, Echchilali K, et al. (2024) Epidermodysplasia Verruciformis: Uncommon Skin Manifestation Unveiling Primary Immunodeficiency. J Case Rep Med Hist 4(3): doi https://doi.org/10.54289/JCRMH2400111
>Copyright : © 2024 Mourabit S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Case Report | Open Access | Full Text
1Resident Physician, Department of Internal Medicine, Ibn Rochd University Hospital, Casablanca, Morocco
2Professor in the Department of Internal Medicine at the Ibn Rochd University Hospital in Casablanca, Morocco
*Corresponding author: Safaa Mourabit, Resident Physician, Department of Internal Medicine, Ibn Rochd University Hospital, Casablanca, Morocco
Abstract
Epidermodysplasia verruciformis (EV) is a rare genetic disorder marked by heightened susceptibility to persistent skin infections caused by human papillomaviruses (HPV). In some instances, EV is associated with immune deficiencies, especially those affecting cellular and humoral responses. Individuals with deficiencies in cellular immunity are more prone to developing EV. This clinical case presents an unusual form of combined immune deficiency, revealed through EV (Lutz-Lewandowsky syndrome). The patient's presentation with extensive verrucous lesions from a young age poses diagnostic challenges. Recurrent respiratory and digestive infections, without other systemic manifestations, complicate the diagnostic process. Decreased lymphocyte subpopulations, including global T, B, and NK lymphopenia, suggest combined immunodeficiency, reinforced by first-degree consanguinity. Negative results in viral serologies and investigations for systemic lupus erythematosus emphasize the importance of considering primary immunodeficiencies. Therapeutic interventions, such as immunoglobulin courses and local laser sessions, demonstrate a multidisciplinary strategy targeting both immune function and cutaneous manifestations. This case underscores the significance of early detection of combined immunodeficiencies for timely intervention and improved patient outcomes. Further research is crucial to explore the genetic complexities of combined immunodeficiencies and their implications in skin disorders like EV.
Keywords: Epidermodysplasia Verruciformis (EV); Immunodeficiency; Global Lymphopenia of T; B and NK Lymphocytes; Human Papillomaviruses (HPV)
Abbreviations: EV: Epidermodysplasia verruciformis, HPV: human papillomaviruses
Introduction
Combined immunodeficiency is a severe hereditary immune deficiency characterized by deficits in humoral and cellular immunity, displaying significant phenotypic heterogeneity. This report details an atypical form marked by EV (Lutz-Lewandowsky syndrome), a rare genetically originated skin condition. Anomalous sensitivity to papillomaviruses leads to anarchic cutaneous horn growth, typically beginning between ages 4 and 8. First described by Felix Lewandowsky and Wilhelm Lutz9, this condition, often referred to as "tree man disease," affects approximately 200 individuals, resulting in scaly macules and pseudo-tumoral papules, predominantly on hands and feet.
Case Report
A 19-year-old patient, born to first-degree consanguineous parents, presented warty lesions since age 10 with a raised and flat appearance, variably hyperpigmented and achromic, covering the entire body (figure 1). Accompanied by recurrent respiratory and digestive infections, there were no other joint, cutaneous-mucosal, or additional manifestations. Biological assessment indicated leukopenia (3160/mm³) and significant lymphopenia (430/mm³). Viral serologies for HIV, HSV, CMV, and EBV were negative. Investigations for systemic lupus erythematosus, including ANA and AC anti-DNA, were negative. Despite digestive symptoms, there were insufficient clinical and biological elements for specific diagnoses such as exudative enteropathy or chronic inflammatory bowel disease. The collapse in lymphocyte subpopulations included global T (CD4 and CD8), B, and NK lymphopenia. Protein electrophoresis revealed no hypogammaglobulinemia, and the weight dosage of immunoglobulins (IgA, IgG, IgM, IgE) was normal, along with a normal DHR test. Considering the opportunistic appearance of warty skin lesions at a young age and first-degree consanguinity, a late-revealed combined immunodeficiency was strongly suspected. Therapeutically, immunoglobulin courses and local laser sessions were indicated.
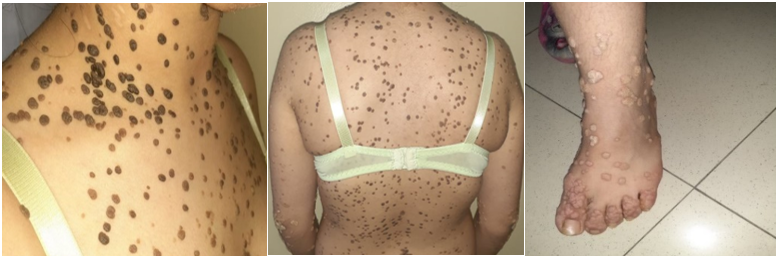
Figure 1: Elevated and flat verrucous lesions, hyperpigmented in some areas and achromic in others, hyperkeratotic, extending over the entire body.
Discussion
In 2018, Huang et al. [1] proposed a new classification of epidermodysplasia verruciformis (EV)into three categories based on presumed cause: classical genetic (EV), non-classical genetic EV and acquired EV (AEV). Classical genetic EV includes mutations in the EVER1/TMC6 and EVER2/TMC8 genes, which play a role in cell-mediated immunity against human papillomavirus (HPV) infection [1,2]. Non-classical genetic VAE includes mutations in several other genes, including RHOH, MST-1, CORO1A and ECM1, of certain HPV types due to impaired cell-mediated immunity [1]. AEV is an EV-like syndrome found secondarily in immunosuppressed states, including HIV and iatrogenic immunosuppression such as organ transplantation [1]. AEV was first reported in case studies in the late 1970s and early 1980s in AIDS patients [3]. In February 2009, Rogers et al. [4] introduced the term acquired VE to describe VE in immunocompromised hosts. AEV was rapidly associated with cutaneous squamous cell carcinomas altered by HPV-5 and HPV-8 DNA sequences [2].
This case presents a rare manifestation of combined immunodeficiency, unveiling itself through epidermodysplasia verruciformis (EV), commonly known as Lutz-Lewandowsky syndrome. The atypical nature of this condition, characterized by anarchic cutaneous horn growth due to abnormal papillomavirus sensitivity, emphasizes the phenotypic diversity within combined immunodeficiencies.
The patient's clinical presentation, with widespread hyperpigmented and achromic warty lesions beginning at an early age, raises diagnostic challenges. The associated respiratory and digestive infectious episodes, in the absence of other systemic manifestations, further complicate the diagnostic process. The collapse in lymphocyte subpopulations, including global T, B, and NK lymphopenia, points toward a combined immunodeficiency, substantiated by first-degree consanguinity. The negative results in viral serologies, systemic lupus erythematosus investigations, and other differential diagnoses highlight the importance of considering primary immune deficiencies, especially when faced with opportunistic infections and consanguinity. The therapeutic approach, involving immunoglobulin courses and local laser sessions, showcases a multidisciplinary strategy targeting both immune function and skin manifestations This case underscores the significance of early detection of combined immunodeficiency, enabling timely intervention and improving patient outcomes. Further research is warranted to explore the genetic intricacies of combined immunodeficiencies and their specific implications in skin disorders such as EV.
Conclusion
This case illustrates a unique form of primary immune deficiency unmasked by EV. Recent genetic discoveries implicate several genes, particularly those involving T cell immunity. Immunological factors, such as deficiency in non-specific cellular immunity and specific inhibition of NK cells or the proliferative response of T lymphocytes toward autologous keratinocytes, have been identified.
References
- Huang S, Wu JH, Lewis DJ, et al. (2018) A novel approach to the classification of epidermodysplasia verruciformis. Int J Dermatol. 57: 1344-1350. [PubMed.]
- Myers DJ, Fillman EP. (2019) Epidermodysplasia verruciformis. In Stat Pearls. Stat Pearls Publishing. [PubMed.]
- Prose NS, Von Knebel-Doeberitz C, Miller S, et al. (1990) Widespread flat warts associated with human papillomavirus type 5: a cutaneous manifestation of human immunodeficiency virus infection. J Am Acad Dermatol. 23(5 Pt 2): 978-981. [PubMed.]
- Rogers HD, MacGregor JL, Nord KM, et al. (2009) Acquired epidermodysplasia verruciformis. J Am Acad Dermatol. 60: 315-320. [PubMed.]